Factors contributing to unintended pregnancies among teenage girls in the informal settlement of Mukuru kwa Njenga, Nairobi, Kenya
Judith Akinyi Odede, Nzomo Mwita, Doreen Othero
Corresponding author: Judith Akinyi Odede, Amref International University (AMIU), Nairobi, Kenya 
Received: 18 Jun 2025 - Accepted: 29 Apr 2026 - Published: 30 Apr 2026
Domain: Health education,Public health,Reproductive Health
Keywords: Teenagers, pregnancy, contraception, reproduction, informal settlement
Funding: This work received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
©Judith Akinyi Odede et al. Primary Health Care Practice Journal (ISSN: 3105-7624). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Judith Akinyi Odede et al. Factors contributing to unintended pregnancies among teenage girls in the informal settlement of Mukuru kwa Njenga, Nairobi, Kenya. Primary Health Care Practice Journal. 2026;4:9. [doi: 10.11604/PHCP.2026.4.9.48358]
Available online at: https://www.phcp-journal.org//content/article/4/9/full
Research 
Factors contributing to unintended pregnancies among teenage girls in the informal settlement of Mukuru kwa Njenga, Nairobi, Kenya
Factors contributing to unintended pregnancies among teenage girls in the informal settlement of Mukuru kwa Njenga, Nairobi, Kenya
Judith Akinyi Odede1,&, Nzomo Mwita1, Doreen Othero1,2
&Corresponding author
Introduction: unintended teenage pregnancy remains a critical public health concern, particularly in Africa, where 93% of adolescent pregnancies occur. In Nairobi, 18% of teenage girls are affected, with higher prevalence in informal settlements such as Mukuru Kwa Njenga. This study aimed to explore and analyze the key factors contributing to unintended pregnancies among teenage girls in this setting, focusing on socio-economic conditions, contraceptive knowledge, access to reproductive health services, and substance abuse.
Methods: a cross-sectional mixed methods design was employed, combining both quantitative and qualitative approaches. Using Fisher´s formula and accounting for a 10% non-response rate, a sample size of 424 adolescent girls was determined. Structured questionnaires were administered to 311 participants, yielding a response rate of 73.3%. In-depth interviews were also conducted with girls who had experienced pregnancy. Quantitative data were analyzed using Statistical Package for the Social Sciences (SPSS) Version 24.0, while qualitative data were coded and analyzed with NVivo 9 software.
Results: the study revealed that 62.7% of respondents had experienced unintended teenage pregnancies. Significant predictors identified through logistic regression included lack of discussions about protection (OR=0.044), limited knowledge of contraceptives (OR=51.731), restricted access to contraceptives (OR=0.106), low household income (OR=31.022), low parental education, and substance abuse, particularly alcohol use (OR=17.333). Qualitative findings showed misinformation, access barriers, economic vulnerability, and substance use driving risky sexual behaviour and unintended pregnancy.
Conclusion: unintended teenage pregnancy in Mukuru Kwa Njenga is driven by a complex interplay of limited contraceptive knowledge, poor access to services, socio-economic challenges, and substance abuse. Addressing these factors requires targeted interventions. Improving youth-friendly services, strengthening reproductive health education, and decentralizing services can enhance access and reduce unintended teenage pregnancies. The study highlights the need for further research on gender norms, partner influence, and health system responsiveness.
Unintended teenage pregnancy remains a major public health concern globally, with sub-Saharan Africa bearing over 90% of the global burden [1]. In Kenya, Nairobi County reports an 18% prevalence rate among teenage girls [2,3], with informal settlements like Mukuru Kwa Njenga presenting uniquely high-risk environments characterized by pervasive poverty [4,5], limited access to youth-friendly reproductive health services, inadequate sex education, widespread contraceptive misinformation, high rates of substance abuse, and persistent social stigma. The consequences of these pregnancies are severe, including maternal and infant mortality, school dropout, and the entrenchment of intergenerational poverty [6,7].
Despite existing research at national and regional levels, there remains a significant knowledge gap regarding the interplay of socio-economic, cultural, and service accessibility factors within informal urban settlements, which hinder the development of targeted interventions. Therefore, this study was guided by four research questions examining: the influence of contraceptive knowledge, access to reproductive health services, socio-economic factors, and substance abuse on the occurrence of unintended teenage pregnancies.
The general objective was to investigate the factors contributing to unintended pregnancies among girls aged 13-19 in Mukuru Kwa Njenga, with four corresponding specific objectives. The study's justification lies in its potential to identify significant causal factors and inform policies that boost reproductive health service utilization. The significance of the study includes generating insights for targeted educational campaigns, advocating for youth-friendly health services, informing poverty alleviation policies, and supporting community-based mentorship and counselling programs. The scope focused on teenagers aged 13-19 in Mukuru Kwa Njenga, examining contraceptive knowledge, substance abuse, and socio-economic factors.
The study is guided by a determinants-based conceptual framework, where unintended teenage pregnancy is influenced by contraceptive knowledge, access to reproductive health services, socio-economic factors, and substance abuse [8]. Government policies act as moderating factors, while parental communication and sex education serve as intervening variables shaping adolescents´ awareness and decision-making.
Study design: a cross-sectional study using a mixed methods approach was conducted to determine the causes of unintended teenage pregnancies in the informal settlement of Mukuru Kwa Njenga, Nairobi County. Quantitative and qualitative data were collected concurrently to enable a comprehensive understanding of the contributing factors, enhance efficiency, and allow for triangulation of findings.
Study setting and population: Mukuru Kwa Njenga is one of Nairobi´s largest informal settlements [9], located in Embakasi South Constituency and extending into parts of Makadara and Starehe. It is bordered by major infrastructure such as the Nairobi Industrial Area, Jomo Kenyatta International Airport, and key roads like the Outer Ring Road and Mombasa Road. The settlement comprises multiple villages, including Mukuru Kwa Reuben, Sinai, and Kayaba, and has an estimated population of over 300,000 [10]. Residents primarily rely on informal, low- income jobs due to poverty and limited access to education. The area is marked by poor housing, inadequate sanitation, and limited access to basic services such as clean water, healthcare, and waste disposal. Health services are largely supported by the Mukuru Health Centre and various non-profit initiatives. Mukuru Kwa Njenga also has one of the highest teenage pregnancy rates in Nairobi, accounting for over half of the city´s reported cases [11], underscoring the need for urgent interventions in reproductive health, education, and social welfare. The study targeted teenage girls aged 13 to 19 living in Mukuru Kwa Njenga informal settlement who were either currently pregnant or had previously given birth. While exact figures on teenage pregnancies in the area are unavailable, local observations and sources confirm the presence of young mothers. An estimated 10,116 girls in this age group fall within the study's target category, drawn from a broader population of approximately 87,203 teenage girls in the settlement.
Variables: the study examines unintended pregnancy as the dependent variable, defined as pregnancies that occurred when a woman wanted to become pregnant in the future but not at the time she became pregnant, or one that occurred when she did not want to become pregnant then or at any time in the future. Independent variables include contraceptive knowledge and use, focusing on awareness, access, and behavioral influences; access to reproductive health services, including availability, distance, and provider attitudes; socio-economic status, such as parental education, income, and living conditions; and substance abuse, covering type, frequency, and its influence on risky sexual behavior. Confounders such as age, marital status, and access to youth-friendly services were accounted for in the analysis.
Data resource and measurement
Data collection tool: data were collected using a structured questionnaire containing both closed- and open-ended questions, covering socio-demographic details, reproductive health, education, economic status, and substance abuse. The tool was pre-tested and administered by trained research assistants. Additional qualitative data were gathered through in-depth interviews to complement the findings. Data collection tools were developed internally based on the study objectives. To ensure validity, the tools were reviewed by subject matter experts and pre-tested in a similar setting to enhance clarity and relevance. Reliability was enhanced through the standardization of questions and consistent administration procedures. Research assistants received prior training covering study objectives, ethical considerations, informed consent procedures, administration of questionnaires, and qualitative interviewing techniques, after which close supervision and daily debriefs were conducted during data collection to maintain data quality.
Data collection: data collection included demographic variables such as age, education level, household size, and family income. The data collection tool also captured independent variables, including access to reproductive health services, school attendance, drug and substance use, peer influence, and exposure to gender-based violence. Data were collected using a structured questionnaire, which was pre-tested on a sample drawn from similar informal settlements to ensure clarity and reliability. The questionnaires and the in-depth interviews were administered during face-to-face interviews with eligible study participants. Data cleaning and analysis were also done using SPSS and NVivo to ensure accuracy and consistency.
Sample size: the sampling frame comprised an estimated 10,116 adolescent girls (13-19) in Mukuru Kwa Njenga identified through schools and NGOs. The sample size was determined using Fisher´s formula, as recommended by Fisher et al. (1998), suitable for large populations exceeding 10,000 [12,13]. With a 95% confidence level (Z = 1.96), a 5% margin of error, and an estimated prevalence of 50%, the initial sample size was calculated at 385.
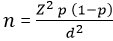
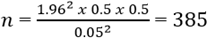
The study employed a combination of purposive and stratified random sampling techniques in the identification of respondents, which was unexpectedly short of the computed sample size by 26.7%. This was largely due to the unwillingness of potential participants to cite personal reasons. Stratified random sampling was applied to ensure proportional representation across eight villages (Riara, Vietnam, Milimani, Wapewape, Motomoto, Sisal, Zone 48, and MCC). Initial identification was done through purposive sampling through schools and NGOs, after which participants were systematically and randomly selected within stratified village clusters to ensure proportional representation. Additionally, respondents for the in-depth interviews were purposively selected based on their knowledge of the study topic, age, and willingness to provide detailed insights. The interviews were conducted until data saturation was attained.
Data analysis: data analysis involved both quantitative and qualitative approaches to provide a comprehensive understanding of the factors contributing to unintended teenage pregnancies. Quantitative data were analyzed using SPSS version 26, with the analysis structured around the study´s specific objectives. Descriptive statistics were used to summarize participant characteristics. Multivariate logistic regression was used to identify independent predictors of unintended teenage pregnancy. All key independent variables aligned to the study objectives: contraceptive knowledge and use, access to reproductive health services, socio-economic factors, and substance abuse, were first examined at the bivariate level. Variables with p ≤ 0.20 at bivariate analysis were included in the multivariate model. Adjusted odds ratios (AORs) with 95% confidence intervals were reported, and statistical significance was set at p < 0.05. Qualitative data from in-depth interviews were analyzed thematically using NVivo software. Interview transcripts were coded to identify recurring patterns, and the resulting themes were categorized according to the study objectives. This thematic analysis aimed to reveal underlying social, cultural, and behavioral influences on teenage pregnancy. The findings from the qualitative data were then integrated with the quantitative results to enrich interpretation and offer a more holistic view of the determinants of unintended teenage pregnancies in Mukuru Kwa Njenga.
Ethical consideration: the study received ethical approval from the Amref Ethics and Scientific Research Committee (ESRC) and was allocated P1384-2023, and a research permit was obtained from the National Commission for Science, Technology and Innovation (NACOSTI) under license number 23/26693. Additional approval was granted by the Ministry of Education. Assent was obtained from participants below the age of 18, along with parental or guardian consent. Participants aged 18 and 19 years provided informed consent directly. Participation in the study was voluntary. Interviews were conducted in private settings due to the sensitive nature of the research topic. To uphold confidentiality, all individuals who interacted with the research data signed a data confidentiality and agreement form. The research team also ensured that information shared during the interviews was not disclosed to third parties.
Out of the 385 targeted respondents, 311 adolescent girls participated, yielding a response rate of 73.3%. The prevalence of unintended teenage pregnancy was 62.7%. Logistic regression analysis identified several significant predictors. Limited knowledge of contraceptives was strongly associated with unintended pregnancy (OR = 51.731), as was lack of protection discussions prior to sexual activity (OR = 0.044), and restricted access to contraceptives (OR = 0.106). Socioeconomic factors such as low household income (OR = 31.022) and lower parental education levels also showed strong associations. Substance abuse, particularly alcohol use, was a notable predictor (OR = 17.333). Additional barriers included fear of stigma, distance to health facilities, irregular operating hours, and negative provider attitudes. Qualitative findings reinforced the quantitative data, revealing recurring themes of misinformation, service inaccessibility, and socio-cultural pressures contributing to adolescent pregnancy.
Model for factors contributing to unintended pregnancy: several factors were significantly associated with unintended pregnancy. Distance to the nearest health facility was a strong predictor, with those living adjacent (OR=0.02, 95% CI: 0.001-0.483) or slightly far (OR=0.004, 95% CI:0-0.081) having significantly lower odds compared to those living very far. Worry about community members discovering contraceptive use significantly increased the odds (OR=18.355, 95% CI: 4.37-77.086). Facility operating hours mattered, as daily availability from 8 AM to 5 PM was protective (OR=0.036, 95% CI: 0.002-0.663) relative to rarely open facilities. Perceived inadequate stock of sexual and reproductive health supplies increased odds (OR=13.724, 95% CI: 1.653-113.919). Access to sex education was protective, with very easy (OR=0.001, 95% CI: 0-0.021) and somewhat easy access (OR=0.036, 95% CI: 0.007-0.187) showing lower odds versus impossible access. Finally, cheerful (OR=0.005, 95% CI: 0-0.085) and calm provider attitudes (OR=0.022, 95% CI: 0.002-0.3) were protective compared to cold attitudes.
Socio-demographic characteristics: most of the respondents' fathers were employed (32.8%), while over half of the respondents´ mothers were self-employed (60.8%). At the time of the study, 22.5% of the mothers were unemployed. Regarding living arrangements, approximately 47% of the respondents lived with both parents, while 20.9% lived with their mothers only (Table 1). The majority of the respondents' fathers had completed primary education, with 17.4% having attained secondary education. In contrast, about 33% of the respondents' mothers had no formal education, while 17.4% and 14.8% had completed secondary and primary education, respectively. Over one-third of the respondents came from households with a monthly income between Ksh. 10,001 and Ksh. 15,000, while 32.5% reported earning less than Ksh. 10,000.
The proportion of teenagers with unintended pregnancy in Mukuru Kwa Njenga was high, with 62.7% of teenage girls reporting at least one unintended pregnancy. Fifty-three point six (53.6%) were aged 16-18 years, while 32.7% came from low-income households earning below Ksh. 10,000 per month. Many had limited education, with only 43.5% reaching secondary level. Although 77.8% were aware of contraceptives, only 34.6% could identify multiple methods correctly, and few discussed protections with partners before sex. Fear of side effects and negative provider attitudes were key barriers to contraceptive use. Access to reproductive health services was limited by irregular facility hours and poor provider attitudes, though availability and positive interactions were protective. Substance use, particularly alcohol and cannabis (locally referred to as bhang), was common and often began before age 13, significantly increasing the risk of unintended pregnancy. Socioeconomic hardship, inadequate reproductive health knowledge, poor service access, and early substance use emerged as major contributing factors.
Contraceptive knowledge and communication: knowledge-related factors emerged as significant determinants of unintended teenage pregnancy. Lack of discussion about protection before sex, limited awareness of contraceptive side effects, and misconceptions about contraceptive effectiveness were associated with higher odds of unintended pregnancy (OR=0.044; 95% CI: 0.011-0.174; p<0.001). Conversely, discussing protection with a partner and having an adequate understanding of contraceptive methods were strongly protective (OR=0.033; 95% CI: 0.003-0.376; p<0.001) (Table 2). Qualitative findings reinforce these results, revealing widespread misinformation, limited parent-adolescent communication, and reliance on peers for sexual health information, all of which contributed to poor contraceptive decision-making. “The fact that I didn´t know how to use the contraceptives put me in danger, which is why I started learning from good sources about them,” a 19-year-old participant reported.
Socio-economic factors: socio-economic conditions significantly influenced unintended teenage pregnancy. Factors such as low household income, low parental education, and unstable living arrangements were associated with increased risk. Adolescents from relatively stable households, including those with civil servant fathers or living with their mothers, had lower odds of unintended pregnancy (OR=0.022; 95% CI: 0.001-0.81; p=0.038) (Table 3). Qualitative findings provide further insight, indicating that economic hardship often drives adolescents into transactional sexual relationships, limiting their ability to negotiate contraceptive use and increasing vulnerability to unintended pregnancy. “Since my dad is jobless, there are times that I have to use some older boys for financial aid, and such situations lead to I can't refuse,” a 16-year-old participant shared.
Substance abuse and risky behavior: substance abuse was a strong predictor of unintended teenage pregnancy. Early initiation of substance use (before age 13), frequent use, and substance use preceding sexual activity were significantly associated with increased risk (OR=3.936; 95% CI: 2.205-7.027; p<0.001). Multivariate analysis further showed that substance use increased the odds of unintended pregnancy more than tenfold (OR=10.102; 95% CI: 2.05-49.79; p=0.004) (Table 4). Use of alcohol and cannabis contributed substantially to the higher risk. Qualitative findings reinforce this relationship, with participants reporting that substance use impaired judgment, reduced contraceptive use, and led to spontaneous, unprotected sexual encounters. “When I am drunk, I completely lose control, and protection is the last thing on my mind,” a 17-year-old participant narrated.
Access to reproductive health services: access to reproductive health services was a key determinant of unintended pregnancy. Limited access to services and information significantly increased the likelihood of unintended pregnancy (OR=18.355; 95% CI: 4.37-77.086; p<0.001), while availability of contraceptives and access to information were strongly protective (OR=0.022; 95% CI: 0.002-0.3; p<0.001) (Table 5). Additional service-related factors, including distance to health facilities, inconsistent availability of supplies, irregular service hours, and negative provider attitudes, were significantly associated with pregnancy outcomes. Fear of stigma from the community further reduced service utilization. These findings are consistent with qualitative reports highlighting structural and psychosocial barriers such as cost, stock-outs, stigma, and lack of privacy. ”It´s expensive to travel such a distance, and I can´t always afford the fare. Consequently, I do not use any birth control methods,” reported a 17-year-old girl. Another narrated that “at times, the clinic has no condoms or contraceptive pills, and I have to do without them”. “I am sometimes anxious that people may eavesdrop on my conversation with the nurse,” a 16-year-old in the IDI said.
The results from the study revealed that unintended teenage pregnancy in Mukuru Kwa Njenga is linked to limited contraceptive knowledge, poor access to reproductive health services, low household income, and substance abuse, with additional contributing factors including inadequate sex education, stigma, and negative attitudes from healthcare providers. The strong association between inadequate knowledge on contraception and unintended pregnancy is consistent with previous studies in sub-Saharan Africa, which show that misinformation, cultural taboos, and limited parent-adolescent communication undermine effective contraceptive use [14-16]. The finding that partner communication is protective aligns with evidence that open discussions enhance negotiation power and contraceptive uptake among adolescents. access to reproductive health services emerged as a critical determinant, with availability of contraceptives and information significantly reducing the likelihood of unintended pregnancy [17]. This supports existing literature emphasizing the role of youth-friendly, accessible services in improving reproductive health outcomes. However, this study further highlights structural and psychosocial barriers such as stigma, provider attitudes, and supply inconsistencies, which are often underemphasized in comparable studies but were strongly evident in both quantitative and qualitative findings.
Socio-economic factors were also significant, reinforcing evidence that poverty, low parental education, and unstable household structures increase vulnerability. The qualitative findings deepen this understanding by illustrating how economic hardship drives transactional relationships, limiting adolescents´ autonomy in reproductive decision-making. Notably, substance abuse emerged as a strong independent predictor, particularly alcohol use, corroborating studies linking substance use to impaired judgment and risky sexual behavior [18,19].
The study used a mixed methods approach, context-specific focus, and robust sample size, providing comprehensive, locally relevant insights, although limitations such as self-reported data, lack of generalizability, and its cross-sectional nature limit causal interpretation. To mitigate limitations, several measures were implemented. Standardized and pre-tested data collection tools were used to enhance validity, while trained research assistants ensured consistency in data collection. The mixed methods design enabled triangulation of findings, strengthening internal validity by complementing quantitative associations with qualitative insights. Although self-reported data may be subject to recall and social desirability bias, confidentiality assurances and appropriate interviewing techniques were employed to minimize these effects. While the cross-sectional design limits causal inference, the use of multivariate analysis helped control for confounding variables. Additionally, although generalizability is limited to similar informal settlement contexts due to the study´s inability to obtain the computed sample size. These findings underscore the urgent need for multi-sectoral interventions that combine sexuality education, improved service delivery, and socio-economic support [20]. However, further research is needed to explore the influence of gender norms, partner dynamics, peer pressure, and the effectiveness of current programs [21,22]. Longitudinal studies and inclusion of male perspectives could provide a more complete understanding of the drivers and potential solutions to adolescent pregnancy in informal urban settings.
The study found a high prevalence of unintended teenage pregnancy in Mukuru Kwa Njenga, with 62.7% of respondents affected. Strong associations were observed with limited contraceptive knowledge, inadequate discussion on protection, misconceptions about side effects, improper use of contraceptives, and restricted access to reproductive health information and services. Structural barriers, including distance to facilities, stigma, limited operating hours, stock-outs, inadequate sex education, and negative provider attitudes, further constrained access. Socio-economic factors such as low household income, parental education, and household structure significantly increased vulnerability. Substance abuse, particularly early initiation and frequent use, also heightened risk through its influence on unsafe sexual behavior. Unintended teenage pregnancy remains a major public health concern in informal settlements. Addressing it requires expanding access to affordable contraceptives, strengthening comprehensive sexuality education, and scaling up youth-friendly services through both facility-based and outreach models. Programs should integrate reproductive health education with substance abuse prevention and improve service quality, including provider attitudes and commodity availability. Community-level efforts should promote parent-adolescent communication, peer education, stigma reduction, and economic empowerment to reduce reliance on transactional relationships. A coordinated, multi-sectoral approach is essential to effectively reduce unintended teenage pregnancies.
What is known about this topic
- High prevalence in low-income settings: teenage pregnancy is a public health issue in many low- and middle-income countries;
- Contraceptive knowledge gaps: the gap in knowledge on contraceptives, including how it works, where to access them, and potential side effects, which contributes to low uptake and inconsistent use;
- Influence of socioeconomic and environmental factors: factors such as parental education, household income, peer influence, and substance abuse are widely recognized as contributors to adolescent sexual behavior and early pregnancy.
What this study adds
- Context-specific insights: the study provides localized evidence on the drivers of unintended teenage pregnancy in Mukuru Kwa Njenga, given the spike of teenage pregnancies, an informal settlement in Nairobi, highlighting the unique socio-economic and environmental challenges faced by teenagers in this setting;
- Integration of quantitative and qualitative data: by combining statistical analysis with in-depth interviews, the study offers a nuanced understanding of how factors such as socio-economic factors, contraceptive knowledge, access to services, and substance abuse interact to influence teenage pregnancy.
- Identification of strong predictors: the research identifies specific high-impact predictors, such as lack of contraceptive discussions and alcohol use, with notably high odds ratios, offering valuable guidance for designing targeted interventions in similar urban informal contexts.
The authors declare no competing interests.
Judith Akinyi Odede was responsible for the overall coordination and execution of the study, including developing the study design, ensuring ethical compliance, obtaining necessary approvals, overseeing data collection and analysis, managing the research team, maintaining data quality and integrity, and preparing reports and publications, also ensured adherence to timelines, budgetary constraints, and regulatory standards. Nzomo Mwita and Doreen Othero provided academic and technical guidance throughout the research process. Their role involved reviewing the study design and tools, offering feedback on data analysis and interpretation, ensuring methodological rigor, and mentoring Judith Akinyi Odede to uphold academic and scientific standards while addressing ethical and practical challenges. All the authors read and approved the final version of this manuscript.
I would like to express my deepest gratitude to the Almighty God for His divine presence and provision throughout this course. I am especially thankful to my supervisors, Dr. Nzomo Mwita and Dr. Doreen Othero, whose invaluable guidance and support made this research possible. I am also profoundly grateful to my husband, Michael Omugah, for constantly encouraging me to step outside my comfort zone and pursue my goals. Additionally, I would like to acknowledge all my mentors, Miss. Yvonne Opanga, Dr. Samuel Muhula, and Mr. Kenneth Juma, whose wisdom and insights have shaped my academic journey. My heartfelt thanks extend to all my lecturers at the School of Postgraduate Studies, Amref International University, as well as my classmates and friends, for their unwavering support and encouragement during my studies. Your contributions have been instrumental in my success.
Table 1: socio-demographic characteristics of teenage girls in Mukuru Kwa Njenga, Nairobi (N=311), July-August 2023
Table 2: association between contraceptive knowledge and unintended teenage pregnancy among adolescent girls in Mukuru Kwa Njenga, Nairobi (n=311), July-August 2023
Table 3: association between socio-economic factors and unintended teenage pregnancy among adolescent girls in Mukuru Kwa Njenga, Nairobi (n=311), July-August 2023
Table 4: association between substance abuse patterns and unintended pregnancy among adolescent girls in Mukuru Kwa Njenga, Nairobi County, Kenya (n=311; July-August 2023)
Table 5: logistic regression of access to reproductive health services and unintended teenage pregnancy among adolescent girls in Mukuru Kwa Njenga, Nairobi (n=311), July-August 2023
- Yakubu I, Salisu WJ. Determinants of adolescent pregnancy in sub-Saharan Africa: a systematic review. Reprod Health. 2018 Jan 27;15(1):15. PubMed | Google Scholar
- Bewa JM. School closures and teenage pregnancy. Bull World Health Organ. 2021 Jan 1;99(1):6-7. PubMed | Google Scholar
- Stats Kenya. Teenage Pregnancy Rates in Kenya by County. Accessed 18th June, 2025.
- Mumah JN, Mulupi S, Wado YD, Ushie BA, Nai D, Kabiru CW et al. Adolescents' narratives of coping with unintended pregnancy in Nairobi's informal settlements. PLoS One. 2020 Oct 29;15(10):e0240797. PubMed | Google Scholar
- Bozzini AB, Bauer A, Maruyama J, Sim�es R, Matijasevich A. Factors associated with risk behaviors in adolescence: a systematic review. Braz J Psychiatry. 2021 Mar-Apr;43(2):210-221. PubMed | Google Scholar
- Nungo S, van Eijk AM, Mason L, Nyothach E, Asuke B, Spinhoven P et al. Factors associated with school dropout and sexual and reproductive health: A cross-sectional analysis among out-of-school girls in western Kenya. BMJ Public Health. 2025 Mar 4;3(1):e001528. PubMed | Google Scholar
- Xavier C, Benoit A, Brown HK. Teenage pregnancy and mental health beyond the postpartum period: A systematic review. J Epidemiol Community Health. 2018 Jun;72(6):451-457. PubMed | Google Scholar
- Theuri J. Influence of community-based ecological interventions on the management of teenage pregnancy in Mombasa County. African Quarterly Social Science Review. 2024;1(1):1. Google Scholar
- UC Berkeley, UON Department of Urban and Regional Planning, Muungano wa Wanavijiji, Slum Dwellers International, Akiba Mashinani Trust, Strathmore University, Katiba Institute. Mukuru Settlement 2017 Situation Analysis: Report Authors. 2017. Accessed 18th June, 2025.
- African Population and Health Research Center (APHRC. Population and Health Dynamics in Nairobi�s Informal Settlements: Report of the Nairobi Cross-sectional Slums Survey (NCSS) 2012. 2014. Accessed 18th June, 2025.
- World Health Organization. Adolescent pregnancy. 2024. Accessed 18th June, 2025
- Fisher AA, Laing JE, Stoeckel JE, Townsend J. Handbook for family planning operations research design.. Population Council. 1998;2. Google Scholar
- Singh AS, Masuku MB. Sampling Techniques and Determination of Sample Size in Applied Statistics Research: An Overview. International Journal of Economics, Commerce and Management. 2014;2(11):1-22.
- Wondimagegne YA, Debelew GT, Koricha ZB. Barriers to contraceptive use among secondary school adolescents in Gedeo zone, South Ethiopia: a formative qualitative study. BMJ Open. 2023 Mar 30;13(3):e060582. PubMed | Google Scholar
- Sarnak DO, Wood SN, Zimmerman LA, Karp C, Makumbi F, Kibira SPS et al. The role of partner influence in contraceptive adoption, discontinuation, and switching in a nationally representative cohort of Ugandan women. PLoS One. 2021 Jan 12;16(1):e0238662. PubMed | Google Scholar
- African Journal of Reproductive Health. Accessed 18th June 2025.
- Harada R, Imoto A, Ndunyu L, Masuda K. The reasons for and influences of unintended teenage pregnancy in Kericho county, Kenya: a qualitative study. Reprod Health. 2024 Oct 8;21(1):143. PubMed | Google Scholar
- Birhanu BE, Kebede DL, Kahsay AB, Belachew AB. Predictors of teenage pregnancy in Ethiopia: A multilevel analysis. BMC Public Health. 2019 May 17;19(1):601. PubMed | Google Scholar
- Connery HS, Albright BB, Rodolico JM. Adolescent substance use and unplanned pregnancy: strategies for risk reduction. Obstet Gynecol Clin North Am. 2014 Jun;41(2):191-203. PubMed | Google Scholar
- Wondimagegne YA, Debelew GT, Koricha ZB. Barriers to contraceptive use among secondary school adolescents in Gedeo zone, South Ethiopia: a formative qualitative study. BMJ Open [Internet]. 2023 Mar 30[cited 2025 Jun 18];13(3):e060582. PubMed | Google Scholar
- Fotso JC, Izugbara C, Saliku T, Ochako R. Unintended pregnancy and subsequent use of modern contraceptive among slum and non-slum women in Nairobi, Kenya. BMC Pregnancy Childbirth. 2014 Jul 10;14:224. PubMed | Google Scholar
- Hadley A. Teenage pregnancy: strategies for prevention. Obstetrics, Gynaecology & Reproductive Medicine. 2020 Dec 1;30(12):387-94. Google Scholar