Prevalence of depression, anxiety, and stress and associated risk factors among young adults in Mathare slums, Nairobi County, Kenya
Grace Wanjugu Kamau, Lucy Njiru, Marion Mutugi, Ann Wamathai
Corresponding author: Grace Wanjugu Kamau, Department of Community Health, School of Public Health, Amref International University, Nairobi, Kenya 
Received: 26 Apr 2025 - Accepted: 21 Apr 2026 - Published: 27 Apr 2026
Domain: Community health,Global health,Health Research
Keywords: Prevalence, mental health challenges, risk factors, young adults, slums, Mathare
Funding: This work received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors
©Grace Wanjugu Kamau et al. Primary Health Care Practice Journal (ISSN: 3105-7624). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Grace Wanjugu Kamau et al. Prevalence of depression, anxiety, and stress and associated risk factors among young adults in Mathare slums, Nairobi County, Kenya. Primary Health Care Practice Journal. 2026;4:5. [doi: 10.11604/PHCP.2026.4.5.47717]
Available online at: https://www.phcp-journal.org//content/article/4/5/full
Research 
Prevalence of depression, anxiety, and stress and associated risk factors among young adults in Mathare slums, Nairobi County, Kenya
Prevalence of depression, anxiety, and stress and associated risk factors among young adults in Mathare slums, Nairobi County, Kenya
![]() Grace Wanjugu Kamau1,&, Lucy Njiru2, Marion Mutugi3, Ann Wamathai4
Grace Wanjugu Kamau1,&, Lucy Njiru2, Marion Mutugi3, Ann Wamathai4
&Corresponding author
Introduction: mental health is a growing global concern, particularly among young adults, with depression, anxiety, and stress accounting for 16% of their morbidity. In Kenya´s urban slums, where young adults comprise 56% of the population, risks are amplified by poverty, unemployment, and violence. Despite high rates of depression (20%) and anxiety (34%) reported in such settings, data specific to Mathare slums remain limited. This study assessed the prevalence and risk factors of mental health conditions among young adults in Mathare, Nairobi County.
Methods: a cross-sectional survey involving 405 participants aged 18-29 years was conducted using convenience sampling. Data were collected through self-administered socio-demographic questionnaires and the depression, anxiety, and stress scale-21 (DASS-21) questionnaire. Descriptive statistics, Pearson´s chi-square tests, and multivariable logistic regression were used for analysis (p < 0.05), conducted with IBM SPSS version 29.0.2.0.
Results: a total of 404 respondents participated (99.8% response rate), with a mean age of 23.2 years. Most were female (69.3%), unemployed (60.4%), and had secondary education (71.5%). The prevalence of depression, anxiety, and stress was 32.2%, 43.1%, and 32.2%, respectively. Bivariate analysis showed that gender (χ2 = 19.152, p < 0.001), employment status (χ2 = 19.379, p < 0.001), income (χ2 = 30.572, p < 0.001) and COVID-19-related income changes (χ2 = 37.252, p < 0.001) were significantly associated with depression and stress. Anxiety was significantly associated with age (χ2 = 11.371, p = 0.016), gender (χ2 = 8.053, p = 0.015), employment status (χ2 = 32.123, p < 0.001), income (χ2 = 26.377, p < 0.001) and COVID-19-related income changes (χ2 = 17.851, p < 0.001). Gender and income level predicted depression and stress, while stable income during the pandemic was protective.
Conclusion: mental health issues, particularly anxiety, were prevalent among young adults in Mathare. Targeted interventions, improved access to care, mental health education, and economic empowerment are urgently needed.
Mental health is a critical global concern due to its significant contribution to morbidity, particularly affecting low- to middle-income countries [1]. The 2019 global burden of disease study highlighted mental health disorders as major contributors to years lived with disability (YLD) globally, with mood and anxiety disorders notably impacting people's well-being and productivity. Among those most impacted are adolescents and young adults, with psychological conditions accounting for 15% of their morbidity [2], prominently featuring stress, anxiety, and depression.
Depression, also known as major depressive disorder, afflicts 264 million individuals worldwide, with a higher prevalence among females [3]. Among young adults, prevalence rates range from 3.5% to 40.8% [4-6]. Anxiety disorders, affecting approximately 301 million people globally, are more prevalent in females [7]. Among young adults, the global prevalence of anxiety increased significantly, with a 52% rise between the year 1990 and 2021 [8]. Stress affects young adults globally, with a prevalence of 35.1% and higher rates in females [9].
Early adulthood, spanning ages 18 to 29 [10], is a transitional phase from adolescence to adulthood, encompassing personal, social, and professional changes. Globally, young adults represent approximately 23% of the population, totaling around 1.8 billion individuals [11]. The transition to adulthood brings challenges like changing living arrangements, social networks, and responsibilities, increasing psychological distress [12]. Academic and professional pressures, alongside financial stressors such as student debt and job insecurity, elevate stress, anxiety, and depression while limiting access to psychiatric care [13,14].
Urban slums in low- and middle-income countries (LMICs) house a growing low-income population in overcrowded, poorly constructed settlements lacking proper infrastructure [15]. Currently, about 1 billion people live in informal settlements, a figure projected to reach 3 billion by 2030 [16,17]. In South East Asia, approximately 31% of urban dwellers reside in slums [18]. India, known for its substantial urbanization, hosts a significant proportion of urban slum residents, with about 17.4% of its urban population, or approximately 65 million people, living in slums [19]. Notably, within these slum communities, young adults constitute a considerable segment of the population, representing roughly 35% of residents in LMICs [20]. In LMICs, 25% of urban dwellers reside in slums, with sub-Saharan Africa experiencing particularly high numbers [21]. Across Kenya, approximately 56% of people living in urban areas reside in informal settlements, with young individuals making up a significant portion of this population [22]. Nairobi's slums, for instance, are home to 33% of young adults aged 18-24 [23]. This demographic confronts issues such as poverty, unemployment, resource scarcity, social exclusion, contact with violent behaviors, and limited availability of community support systems [24], all of which contribute to heightened depressive symptoms [25]. An estimated 60% to 80% of people living in urban areas in Nairobi reside in informal settlements [26]. While informal settlements occupy just 5% of the total land area in Nairobi, they house over half of the city's population [27].
In Kenya´s urban informal settlements, the occurrence of anxiety and depressive disorder among young adults was 20% and 34% repectively [28]. Mathare slums, the oldest informal settlement in Nairobi, Kenya´s capital, have been confronted with various social and health challenges, including cholera outbreaks, gang violence, and building collapses, all of which can be attributed to inadequate and unregulated development [29]. A significant portion of the slum lacks access to clean drinking water, with many areas not connected to the municipal water supply. Additionally, the absence of proper sewer lines has resulted in the discharge of wastewater from tall buildings directly into nearby rivers, exacerbating the sanitation issues within the community [29]. The young adults residing in Mathare slums encounter distinctive challenges that have the potential to influence their mental well-being. These challenges encompass limited access to fundamental services such as healthcare and education, pervasive poverty, high unemployment rates, prevalent crime, and violence. As a result, these difficulties can exacerbate stress levels and contribute to heightened anxiety and depression among individuals.
The majority of the LMICs face neglected policy attention when it comes to mental wellness, resulting in significant budgetary gaps and understaffing dedicated to mental wellness services. According to Jaguga et al. [30], Kenya confronts a critical shortage of psychiatric care facilities and professionals. For instance, there is a scarcity of psychiatric care facilities and a significant scarcity of mental health professionals. Specifically, the psychologist-to-population ratio is alarmingly high, estimated at 1 psychologist for every 4.6 million individuals. Furthermore, the accessibility of psychiatric care in the public sector in Kenya is extremely limited, with less than 1% offering such services.
With the inadequate mitigative measures, the young adults in Mathare slums are more exposed to mental disorders. A substantial body of literature on psychological health in Kenya has paid special attention to the general population. However, data on mental health prevalence in specific slums, such as Mathare, remains limited, posing challenges for tailored interventions. The absence of such crucial information hampers policymakers and healthcare providers in attending to the mental health concerns of these communities. This study, therefore, aims to assess the prevalence of depression, anxiety, and stress and examine the associated risk factors among the young adults in Mathare slums, Nairobi County, Kenya.
Study design: a cross-sectional study was conducted to assess the prevalence of depression, anxiety, and stress along with their associated risk factors, among young adults living in the Mathare slums of Nairobi, Kenya.
Study setting: the research was undertaken in Mathare slums, positioned 5 -10 kilometers northeast of Nairobi's Central Business District. Spanning approximately 3 square kilometers, this densely populated area is home to 206,564 individuals with an almost equal ratio of males to females [31]. Mathare slum, located in the Mathare Sub-County, comprises five sub-locations: Huruma, Kiamaiko, Mlango Kubwa Mathare, Mabatini, and Hospital. As the oldest informal settlement in Nairobi City County, Mathare is characterized by its high population density. With a staggering 68,941 residents per square kilometer, it far exceeds the national average of 82 persons per square kilometer [29]. Data collection occurred from January to February 2024.
Participants: this study focused on young adults in the 18-29 age cohort residing within Mathare slums. A sample of 405 participants was recruited using a convenience sampling approach from a health center within Mathare Constituency. Eligible participants were approached in person by trained research assistants, who provided information about the study and invited them to participate through self-administered questionnaires. To be included in this study, the participants had to satisfy the following inclusion criteria: (1) belong to the 18-29 years old category; (2) be a resident of Mathare slums; (3) be able to comprehend English and Kiswahili; and (4) provide written consent indicating their willingness to participate.
Variables: the predictor variables under study include age, gender, educational attainment, employment status, income range per month, marital status, and household income affected by COVID-19, while the outcome variables are depression, anxiety, and stress.
Variables measurement: two questionnaires were used: a semi-structured questionnaire for socio-demographic data (age, gender, education, occupation, income, marital status and other household characteristics) and the 21-item Depression Anxiety and Stress Scale (DASS-21) to assess mental health [32]. DASS-21 uses a 4-point scale, with scores in each subscale doubled to match the full DASS-42. Higher scores indicate greater severity. Depression scores were categorized as normal (0-9), mild (10-13), moderate (14-20), severe (21-27) and extremely severe (28+); anxiety: normal (0-7), mild (8-9), moderate (10-14), severe (15-19) and extremely severe (20+); and stress: normal (0-14), mild (15-18), moderate (19-25), severe (26-33) and extremely severe (34+).
Sample size: sample size calculation was performed using the Daniel sample size formula [33] to calculate the adequate sample population for prevalence research.
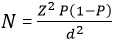
Where N is the required sample population; Z2 is 1.96 at 95% confidence interval; P is the expected prevalence, which was estimated at 0.5, and d is the estimated acceptable error margin for proportion (0.05). This gave N = 385. A sample size of 405 was obtained after adjusting the initially calculated sample size (N) to account for a 5% loss using the formula to N adj=N/(1-5% loss). This is to ensure that the potential loss of data in the calculation of the final sample size is incorporated.
Statistical analysis: data were collated in Excel and analyzed using IBM SPSS version 29.0.2.0 (20) free trial. Descriptive results were reported as percentages and means. Depression, anxiety, and stress were classified as present or absent based on cut-off scores and analyzed across demographic groups. Predictor variables (age, gender, education, employment, income, marital status and COVID-19-related income impact) were categorized. Variables such as income, which had missing responses, likely due to its sensitive nature, were retained and categorized as non-response to minimize data loss and potential bias associated with complete case analysis. Associations were assessed using Pearson´s Chi-square tests, and significant predictors underwent multivariable logistic regression to calculate adjusted odds ratios with 95% confidence intervals. A p-value < 0.05 indicated statistical significance.
Ethical considerations: ethical approval for this study was granted by the Amref Ethics and Scientific Review Committee (ESRC), under approval number AMREF-ESRC P1558/2023. All participants provided written informed consent, and the study complied with ethical standards in accordance with the Helsinki Declaration.
Socio-demographic characteristics: data from 404 eligible participants (99.8% response rate) were analyzed. The mean age was 23.2 years, with a predominance of females (69.3%). On education, 99.2% of the participants had formal education, with 71.5% having secondary education. While 39.4% reported having some form of employment, the majority were either unemployed (60.4%) or in informal work, including self-employment (23.5%) and casual labor (6.7%). Only 42.2% had an income, with a majority earning less than KES 10,000 monthly. The majority were married (54.2%), and 29.7% reported that their household income had been negatively impacted by COVID-19, citing job loss, pay cuts, and reduced business (Table 1).
Prevalence and severity levels of the mental disorders: depression, anxiety and stress affected 32.2%, 43.1%, and 32.2% of participants, respectively. Moderate levels were most common-16.1% for depression and stress, while 20.0% for anxiety. Mild cases were also notable, with 10.9% for both depression and stress and 14.6% for anxiety. Severe and extremely severe forms were less frequent, each affecting fewer than 3% of participants (Table 2).
Distribution of mental disorders by their socio-demographic characteristics: depression and stress were most prevalent among individuals aged 24-26 years (36.8%) and were significantly more common in males than females (36.0% vs. 28.2%; p < 0.001). Higher education levels were linked to increased prevalence of depression and stress, with 42.7% of undergraduates and 45.5% of postgraduates affected. Those in casual employment (59.3%; p < 0.001) and earning between KES 31,000-40,000 monthly (75%; p < 0.001) were significantly associated with higher depression and stress levels. On marital status, depression and stress were highest among divorcees (100%), and individuals from households financially affected by COVID-19 also reported significantly higher rates of depression and stress (50%; p < 0.001). Bivariate analysis summarizing the factors associated with prevalence of depression and stress revealed significant associations with gender (χ2 = 19.152, df = 2, p < 0.001), employment status (χ2 = 19.379, df = 4, p < 0.001), income (χ2 = 30.572, df = 6, p < 0.001) and COVID-19-related income disruption (χ2 = 37.252, df = 2, p < 0.001). No significant associations were found with age, educational attainment, or marital status.
Anxiety was significantly higher among individuals aged 21-23 years (49.2%) and was significantly greater in males than in females (50.50% vs 38.90%; p=0.015). On educational attainment, persons with undergraduate studies were more anxious; part time or casual employees had significantly higher levels of anxiety (81.50%; p< 0.001); high income earners (those earning between KSH 31,000-40,0000 per month) showed significantly higher levels of anxiety (75%; p < 0.001); divorcees had higher levels of anxiety (100%) and households whose income was not affected by COVID-19 showed significantly higher levels of anxiety (46.10%; p < 0.001). Bivariate analysis summarizing the factors associated with prevalence of anxiety showed that age ( χ2 =11.371, df= 4, p=0.016), gender (χ2 =8.053, df= 2, p=0.015), employment status (χ2 = 32.123, df=4, p < 0.001), income range per month (χ2 = 26.377, df=6, p < 0.001) and household income affected by COVID-19 (χ2 = 17.851, df=2, p < 0.001) had significant associations with anxiety while educational attainment and marital status did not show significant associations (Table 3).
Multivariate analysis to predict depression, anxiety, and stress: multivariable logistic regression was used to determine the significant predictors of depression, anxiety, and stress among young adults residing in the Mathare slums. The findings from this analysis revealed that gender played a significant role in predicting depression and stress, but not anxiety. Specifically, males exhibited significantly lower odds of experiencing depression and stress compared to females (AOR = 0.150, 95% CI: 0.028-0.803, p = 0.027), meaning that males were approximately 85% less likely to experience these conditions than females.
Additionally, income levels were identified as a significant predictor of depression and stress. Participants earning less than KES 5,000 per month were found to have significantly elevated odds of experiencing depression and stress in comparison to those in higher income brackets (AOR = 3.69, 95% CI: 1.232-11.060, p = 0.020). This indicates that individuals in the lowest income group were 3.69 times more likely to report depression and stress than those earning more. Furthermore, economic stability during the COVID-19 pandemic emerged as a protective factor against depression and stress. Individuals whose household income remained unaffected by the pandemic had significantly lower odds of experiencing these conditions (AOR = 0.132, 95% CI: 0.038-0.458, p = 0.001) (Table 4).
This study aimed to investigate the prevalence of depression, anxiety, and stress among young adults in Mathare slums, Nairobi County, Kenya, and to explore associated risk factors. The prevalence rates were 32.2% for both depression and stress, and 43.1% for anxiety, figures notably higher than general population estimates, highlighting the increased vulnerability of individuals in informal settlements.
Comparative studies in LMICs reflected similar trends. For instance, a study in Ethiopia reported even higher prevalence rates of depression (41.4%), anxiety (66.7%), and stress (52.2%) [34]. Findings from North-West Tanzania showed comparable levels of depression (36%) and anxiety (31%) [35]. Similarly, research among University of Nairobi students reported moderate to high stress levels ranging from 27.6% to 37.0% [36]. A study conducted during the COVID-19 pandemic in Nairobi County found that approximately 27% of young men and 30% of young women (aged 16-25) exhibited depressive symptoms, while around 38% of both genders showed signs of anxiety [37].
The study revealed notable socio-demographic differences in mental health outcomes. Depression and stress were most prevalent among individuals aged 24-26 (36.8%), while anxiety was highest among those aged 21-23 (49.2%). These findings align with Kessler et al. [38], who found that young adults were particularly vulnerable to mental health issues due to life transitions and stress related to finances, academics, or employment. While age was significantly associated with anxiety, it was not significantly linked to depression or stress.
Gender differences were also observed, with men reporting higher levels of depression, anxiety, and stress, contrary to findings by Seedat et al. [39], who noted higher rates among women. Although women generally experience a higher lifetime prevalence of anxiety, men may experience more severe forms when they do occur [39]. Higher educational attainment was associated with increased depression and stress, particularly among undergraduates (42.7%) and postgraduates (45.5%). This aligned with the study by Eaton et al. [40], who noted that although higher education was typically linked to better physical health and longevity, it was also linked to elevated stress and depression due to academic pressures, career uncertainty and the burden of balancing education with financial or family responsibilities. Anxiety was most prevalent among undergraduates (54.7%) and those with secondary education (41.2%), though overall, educational attainment was not significantly associated with all psychological disorders.
Employment status showed notable disparities. Individuals in casual employment reported significantly high levels of depression (59.3%), anxiety (81.5%), and stress (59.3%), supporting Butterworth et al. [41], who found that precarious employment heightened mental health risks through economic instability, job dissatisfaction, and social exclusion. High-income earners (Ksh 31,000-40,000) reported significantly higher levels of depression, anxiety, and stress (75.0%; p < 0.001). As noted by Marmot et al. [42], income inequality played a key role in mental health; while higher incomes granted better access to resources, they also came with stressors like long hours, competitive work environments and pressure to maintain success, which can contribute to burnout and psychological distress. Marital status also influenced mental health, with divorcees exhibiting the highest rates of depression, anxiety, and stress (100%). Whisman et al. [43] highlighted that divorce increased vulnerability to mental health challenges due to emotional strain, financial stress, and the difficulty of adapting to a new lifestyle. Conversely, supportive marriages acted as protective buffers against mental illness. However, in this study, marital status showed no significant association with psychological disorders.
The impact of COVID-19 was also evident; individuals whose household income was affected reported significantly higher rates of depression (50%), anxiety (38.5%), and stress (50%) (p < 0.001). This aligned with findings by Xiong et al. [44], who reported elevated psychological disorders globally due to pandemic-related stressors such as social isolation, fear of infection, and economic uncertainty. Household income disruptions due to COVID-19 were significantly associated with all three mental health conditions.
Multivariate analysis revealed that gender significantly predicted depression and stress, with males showing lower odds compared to females. This aligned with findings from studies in informal settlements in South Africa [45] and Nakuru County, Kenya [46], which reported higher levels of depression and stress among women. Income level also emerged as a significant determinant of depression and stress. This was supported by evidence from Lund et al. [47], who found that individuals with lower socioeconomic status in LMICs were more prone to mental disorders. Similarly, research in Kenya, such as in Migori County, observed a dose-response relationship between poverty and depressive symptoms [48]. Moreover, economic stability during the COVID-19 pandemic significantly reduced the risk of depression and stress. Those whose household incomes were unaffected had lower odds of experiencing these issues, echoing findings by Kola et al. [49], who linked pandemic-related economic instability to increased mental health disorders in LMICs.
Strengths and limitations: this study has several notable strengths. The use of the DASS-21, a validated and widely applied instrument, enhances the reliability of assessing depression, anxiety, and stress. A relatively high response rate reduces the risk of non-response bias and improves sample representativeness. Additionally, the focus on a vulnerable and under-researched population provides valuable insights into an often-overlooked context.
However, some limitations should be considered. The reliance on self-reported data may introduce social desirability and recall bias, potentially affecting accuracy. The focus on young adults and the study´s restriction to a single urban informal settlement in Kenya limit generalizability. The observed gender imbalance, with a higher proportion of female participants, may introduce bias by limiting the representativeness of the study population and leading to biased effect estimates if not properly adjusted for in the analysis. Furthermore, the use of convenience sampling may have introduced selection bias and limited the generalizability of the findings, and the use of a cross-sectional design, as well as the absence of follow-up, limits the ability to assess changes over time or establish causal relationships.
The study revealed a high prevalence of moderate to severe symptoms of depression, anxiety, and stress among young adults. Mental health outcomes varied significantly across socio-demographic and economic factors, including age, gender, education, employment, income, marital status, and COVID-19-related financial disruptions. Bivariate analysis showed significant associations between mental health outcomes and several factors, including age, gender, employment, income, and COVID-19 impact. However, in multivariable analysis, gender, income, and financial stability remained significant predictors. Males were less likely to experience depression and stress after adjusting for confounders, while lower income was associated with increased mental health risks. Stable income during the COVID-19 period appeared to be protective. These findings point to the need for a comprehensive approach to mental health among young adults in Mathare. Strengthening surveillance, early intervention, and access to information can help reduce psychological disorders and address group-specific disparities. Integrating mental health into existing healthcare systems and developing tailored strategies based on age, gender, education, employment, income, and marital status are essential. Providing well-paying job opportunities can alleviate economic strain. Additionally, promoting mental health literacy can empower individuals to manage their own well-being and support others.
What is known about this topic
- Mental health conditions are widespread among young adults worldwide, particularly in low- and middle-income nations, where the availability of mental health care is often inadequate;
- Living in poverty and facing socio-economic hardships are major contributors to the development of mental health issues like depression, anxiety, and stress, especially for individuals residing in underserved urban settlements;
- The COVID-19 pandemic intensified psychological distress, with higher instances of depression, anxiety and stress linked to financial instability, social disconnection, and the unpredictability of life circumstances.
What this study adds
- This research centers on individuals aged 18 to 29, a pivotal period identified by the WHO (2021) as early adulthood, characterized by significant personal, social, and career-related transformations; these transitions can heighten susceptibility to mental health issues, making this age group particularly vulnerable yet often underrepresented in mental health discourse;
- The study delivers context-specific evidence on the rates of depression, anxiety, and stress among young adults residing in Mathare, an informal settlement in Nairobi; it enriches the scarce but expanding research base on mental health conditions within urban slums in Kenya and across the sub-Saharan region;
- Furthermore, it highlights critical socio-demographic and economic predictors, including gender, employment status, and financial stability during the COVID-19 crisis, that are significantly linked to mental health outcomes; these findings offer valuable guidance for the development of tailored, age-appropriate mental health programs for youth in marginalized and resource-limited communities.
The authors declare no competing interests.
Conceptualization: Grace Wanjugu Kamau, Lucy Njiru, Marion Mutugi, and Ann Wamathai; methodology: Grace Wanjugu Kamau, Lucy Njiru, and Marion Mutugi; data collection: Grace Wanjugu Kamau, and Ann Wamathai; formal analysis: Grace Wanjugu Kamau, Lucy Njiru, and Marion Mutugi; resources: Grace Wanjugu Kamau and Ann Wamathai, writing-original draft preparation: Grace Wanjugu Kamau and Lucy Njiru; writing-review and editing Grace Wanjugu Kamau, Lucy Njiru, and Marion Mutugi; and Ann Wamathai; supervision: Lucy Njiru and Ann Wamathai. All the authors read and approved the final version of this manuscript.
The author would like to express sincere gratitude to the third and fourth authors for their invaluable contributions to the design of the study, data acquisition, and constructive feedback during the analysis and interpretation stages. Their insights and critical review of the manuscript significantly enriched the quality of this work. The author would also like to thank the participants for their involvement in the study and their support in facilitating the fieldwork during the research period.
Table 1: demographic characteristics of study participants, recruited from Mathare slums (Nairobi, Kenya), aged 18-29 years, from January to February 2024 (N = 404)
Table 2: prevalence and severity levels of depression, anxiety, and stress among of study participants, recruited from Mathare slums (Nairobi, Kenya), aged 18-29 years
Table 3: distribution of mental disorders by their socio-demographic characteristics among young adults in Mathare slums (Nairobi, Kenya)
Table 4: multivariate analysis of variables associated with depression, anxiety, and stress among young adults (18-29 years) of Mathare Slums, Nairobi
- Moitra M, Owens S, Hailemariam M, Wilson KS, Mensa-Kwao A, Gonese G et al. Global Mental Health: Where We Are and Where We Are Going. Curr Psychiatry Rep. 2023 Jul;25(7):301-311. PubMed | Google Scholar
- World Health Organization. Mental health of adolescents. 2025. Accessed 26th April, 2025.
- World Health Organization. Depressive disorder (depression). 2025. Accessed 29th April, 2026.
- Auerbach RP, Alonso J, Axinn WG, Cuijpers P, Ebert DD, Green JG et al. Mental disorders among college students in the World Health Organization World Mental Health Surveys. Psychol Med. 2016 Oct;46(14):2955-2970. PubMed | Google Scholar
- Oladeji BD, Bello T, Kola L, Araya R, Zelkowitz P, Gureje O. Exploring Differences Between Adolescents and Adults With Perinatal Depression-Data From the Expanding Care for Perinatal Women With Depression Trial in Nigeria. Front Psychiatry. 2019 Oct 24;10:761. PubMed | Google Scholar
- Gustavson K, Knudsen AK, Nesv�g R, Knudsen GP, Vollset SE, Reichborn-Kjennerud T. Prevalence and stability of mental disorders among young adults: findings from a longitudinal study. BMC Psychiatry. 2018 Mar 12;18(1):65. PubMed | Google Scholar
- Javaid SF, Hashim IJ, Hashim MJ, Stip E, Samad MA, Ahbabi AA. Epidemiology of anxiety disorders: global burden and sociodemographic associations. Middle East Curr Psychiatry. 2023;30(1):44. Google Scholar
- Bie F, Yan X, Xing J, Wang L, Xu Y, Wang G et al. Rising global burden of anxiety disorders among adolescents and young adults: trends, risk factors, and the impact of socioeconomic disparities and COVID-19 from 1990 to 2021. Front Psychiatry. 2024 Nov 26;15:1489427. PubMed | Google Scholar
- Smith MD, Wesselbaum D. Global evidence on the prevalence of and risk factors associated with stress. J Affect Disord. 2025 Apr 1:374:179-183. PubMed | Google Scholar
- Arnett JJ, �ukauskiene R, Sugimura K. The new life stage of emerging adulthood at ages 18-29 years: implications for mental health. Lancet Psychiatry. 2014 Dec;1(7):569-76. PubMed | Google Scholar
- The Commonwealth. The Global Picture. Accessed 19th April, 2026.
- Arnett JJ. Emerging adulthood: A theory of development from the late teens through the twenties. Am Psychol. 2000 May;55(5):469-80. PubMed | Google Scholar
- Abrams Z. Student mental health is in crisis. Campuses are rethinking their approach. Last updated: October 12, 2022. 2022. 19th April, 2026.
- Geiman J. The Psychological Toll of Student Debt. Accessed 19th April, 2026.
- Human Settlements Programme United Nations. The Millennium development goals and urban sustainability: 30 years of shaping the Habitat Agenda. 2006.
- United Nations. World Population Prospects 2019: Highlights. 2019.
- United Nation-Habitat. GLOBAL ACTION PLAN: Accelerating for Transforming Informal Settlements and Slums by 2030. Accessed 26th April, 2025.
- Minnery J, Argo T, Winarso H, Hau D, Veneracion CC, Forbes D et al. Slum upgrading and urban governance: Case studies in three South East Asian cities. Habitat Int. 2013;39:162-169. Google Scholar
- Kumar P. Slums in India: Results from Census. Journal of Environmental and Social Sciences. 2011.
- Ssemugabo C, Nalinya S, Lubega GB, Ndejjo R, Musoke D. Health risks in our environment: Urban slum youth�perspectives using photovoice in Kampala, Uganda. Sustainability. 2020 Dec 29;13(1):248. Google Scholar
- United Nation-Habitat. World Cities Report 2020: The Value of Sustainable Urbanization. 2020.
- Muthomi K. New report stresses need for slum upgrade program in urban areas. Capital Business. 2024. Accessed 24th April, 2025.
- Wa Teresia JN. Juvenile Delinquency and Crime Nairobi Slum Areas, Kenya. East Afr J Arts Soc Sci. 2021;4(1):22-38.
- Muiya BM. The Nature, Challenges and Consequences of Urban Youth Unemployment: A Case of Nairobi City, Kenya. Universal journal of educational research. 2014;2(7):495-503. Google Scholar
- Khasakhala LI, Ndetei DM, Mutiso V, Mbwayo AW, Mathai M. The prevalence of depressive symptoms among adolescents in Nairobi public secondary schools: association with perceived maladaptive parental behaviour. Afr J Psychiatry (Johannesbg). 2012 Mar;15(2):106-13. PubMed | Google Scholar
- Amendah DD, Buigut S, Mohamed S. Coping strategies among urban poor: evidence from Nairobi, Kenya. PLoS One. 2014 Jan 10;9(1):e83428. PubMed | Google Scholar
- Da Cruz F. Nairobi Urban Sector Profile. UN-HABITAT. 2006. Google Scholar
- Angwenyi V, Kabue M, Chongwo E, Mabrouk A, Too EK, Odhiambo R et al. Mental Health during COVID-19 Pandemic among Caregivers of Young Children in Kenya's Urban Informal Settlements. A Cross-Sectional Telephone Survey. Int J Environ Res Public Health. 2021 Sep 25;18(19):10092. PubMed | Google Scholar
- Kariuki J. Mathare slums most congested area with 68,941 per square kilometre. 2020. Accessed 24th April, 2025.
- Jaguga F, Kwobah E. Mental health response to the COVID-19 pandemic in Kenya: a review. Int J Ment Health Syst. 2020 Aug 18:14:68. PubMed | Google Scholar
- Kenya R. Kenya population and housing census. 2019.
- DASS-21 Scoring template and interpretation. Accessed 16th April, 2026.
- Daniel WW, Cross CL. Biostatistics: a foundation for analysis in the health sciences. John Wiley & Sons. 2018 Nov 13. Google Scholar
- Nakie G, Segon T, Melkam M, Desalegn GT, Zeleke TA. Prevalence and associated factors of depression, anxiety, and stress among high school students in, Northwest Ethiopia, 2021. BMC Psychiatry. 2022 Nov 28;22(1):739. PubMed | Google Scholar
- Kuringe E, Materu J, Nyato D, Majani E, Ngeni F, Shao A et al. Prevalence and correlates of depression and anxiety symptoms among out-of-school adolescent girls and young women in Tanzania: A cross-sectional study. PLoS One. 2019 Aug 16;14(8):e0221053. PubMed | Google Scholar
- Oketch-Oboth JWB, Okunya LO. The Relationship Between Levels of Stress and Academic Performance Among University of Nairobi Students. Int J Learn Dev. 2018;8(4):1. Google Scholar
- Gichangi PB, Byrne ME, Thiongo MN, Waithaka M, Devoto B, Gummerson E et al. Impact of COVID-19 on the mental health of adolescents and youth in Nairobi, Kenya. Front Psychiatry. 2024 Feb 8;14:1209836. PubMed | Google Scholar
- Kessler RC, Berglund P, Demler O, Jin R, Merikangas KR, Walters EE. Lifetime prevalence and age-of-onset distributions of DSM-IV disorders in the National Comorbidity Survey Replication. Arch Gen Psychiatry. 2005 Jun;62(6):593-602. PubMed | Google Scholar
- Seedat S, Scott KM, Angermeyer MC, Berglund P, Bromet EJ, Brugha TS et al. Cross-National Associations Between Gender and Mental Disorders in the World Health Organization World Mental Health Surveys. Arch Gen Psychiatry. 2009 Jul;66(7):785-95. PubMed | Google Scholar
- Eaton WW, Muntaner C, Bovasso G, Smith C. Socioeconomic status and depressive syndrome: the role of inter- and intra-generational mobility, government assistance, and work environment. J Health Soc Behav. 2001 Sep;42(3):277-94. PubMed | Google Scholar
- Butterworth P, Leach LS, Strazdins L, Olesen SC, Rodgers B, Broom DH. The psychosocial quality of work determines whether employment has benefits for mental health: results from a longitudinal national household panel survey. Occup Environ Med. 2011 Nov;68(11):806-12. PubMed | Google Scholar
- Marmot M, Friel S, Bell R, Houweling TA, Taylor S; Commission on Social Determinants of Health. Closing the gap in a generation: health equity through action on the social determinants of health. Lancet. 2008 Nov 8;372(9650):1661-9. PubMed | Google Scholar
- Whisman MA. The association between depression and marital dissatisfaction. 2001. Google Scholar
- Xiong J, Lipsitz O, Nasri F, Lui LMW, Gill H, Phan L et al. Impact of COVID-19 pandemic on mental health in the general population: A systematic review. J Affect Disord. 2020 Dec 1;277:55-64. PubMed | Google Scholar
- Gibbs A, Govender K, Jewkes R. An exploratory analysis of factors associated with depression in a vulnerable group of young people living in informal settlements in South Africa. Glob Public Health. 2018 Jul;13(7):788-803. PubMed | Google Scholar
- Lambert JE, Denckla C. Posttraumatic stress and depression among women in Kenya's informal settlements: risk and protective factors. Eur J Psychotraumatol. 2021 Jan 26;12(1):1865671. PubMed | Google Scholar
- Lund C, Breen A, Flisher AJ, Kakuma R, Corrigall J, Joska JA et al. Poverty and common mental disorders in low and middle income countries: A systematic review. Soc Sci Med. 2010 Aug;71(3):517-528. PubMed | Google Scholar
- Starnes JR, Di Gravio C, Irlmeier R, Moore R, Okoth V, Rogers A et al. Characterizing multidimensional poverty in Migori County, Kenya and its association with depression. PLoS One. 2021 Nov 16;16(11):e0259848. PubMed | Google Scholar
- Kola L, Kohrt BA, Hanlon C, Naslund JA, Sikander S, Balaji M et al. COVID-19 mental health impact and responses in low-income and middle-income countries: reimagining global mental health. Lancet Psychiatry. 2021;8(6):535-550. PubMed | Google Scholar